News
Hepatitis C Virus outbreak among millennials
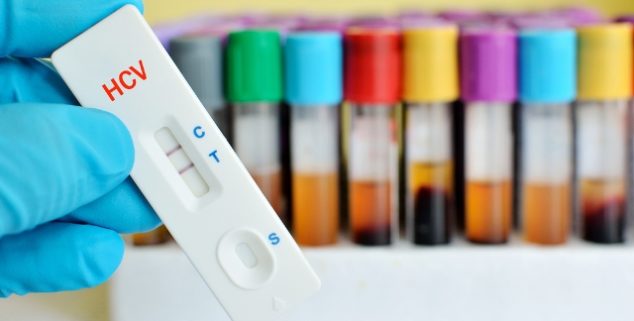 Laboratory testing of HCV. (Photo: Jarun Ontakrai, via Shutterstock)
Laboratory testing of HCV. (Photo: Jarun Ontakrai, via Shutterstock)Millennials haven’t inherited the best batch of goods from baby boomers. They got a housing crisis, a shaky job market, and some enormous student loans.
But until recently, viral hepatitis was the burden of boomers alone to bear. Now, millennials are also facing an outbreak of Hepatitis C Virus (HCV).
There were nearly 2,000 opioid overdose deaths and over 4,000 hospitalizations for opioid overdoses in California in 2015
With existing money tight and future funding uncertain to test and treat hepatitis, the observed increase could be just the tip of the iceberg.
California’s Department of Public Health says newly reported HCV infections increased 55 percent among men aged 20-to-29, from 2007 to 2015. Among women in the same age group the increase was 37 percent.
Viral hepatitis is often thought of as a disease of baby boomers. Since Hepatitis C wasn’t screened out of the blood supply until 1992, it’s been mostly older populations who are affected.
But California is now seeing a spike in new HCV infections in millennials. With existing money tight and future funding uncertain to test and treat hepatitis, the observed increase could be just the tip of the iceberg.
Many public health experts agree that the new cases are a result of an increase in injection drug use.
“Increasing disease in younger people is concerning because it reflects recent disease transmission, likely due to increases in opioid use and injection drug use,” the California Department of Public Health (CDPH) told Capitol Weekly in an email.
Statewide, the rate is 4.73 overdose deaths per 100,000 residents. In some rural counties, the rate is much higher.
California isn’t alone.
According to research published by the Centers for Disease Control, in Kentucky, Tennessee, Virginia and West Virginia, the populations newly infected with HCV are strongly linked to those affected by the opioid crisis: mostly young, white men in rural areas.
“Although drug overdose mortality in California has not increased as dramatically as in other states in recent years, in 2015, 18 counties had an opioid overdose mortality rate at least 50% higher than the statewide average,” CDPH said.
Statewide, the rate is 4.73 overdose deaths per 100,000 residents. In some rural counties, the rate is much higher: Tuolumne and Humboldt had rates as high as 24.69 and 13.76, respectively.
This recent increase in the use of first prescription opioid painkillers and now cheaper and more attainable opioids like heroin has grabbed the nation’s attention.
In 2015, the state Legislature disbursed a $2.2 million, three-year grant for pilot projects to address increasing HCV infections.
But according to health care workers in more urban areas like Katie Burk, the Viral Hepatitis Coordinator for the San Francisco Department of Public Health, injection drug use and its related consequences persist as health issues affecting city populations.
While in rural areas, the narrative of this new surge in opioid use is established, the numerical increase in urban Hepatitis C cases has been small, but the percentage has increased significantly.
“What we’re seeing nationally, everyone is talking about the opioid crisis. That is concentrated among younger, rural or suburban, mostly Caucasian, mostly males,” Burk said. “In San Francisco, our story is a little different … We’ve had a steady incidence of Hepatitis C in younger users here.”
The facilities that treat Hepatitis C are perpetually underfunded, Burk and other public health care professionals agree.
Health care professionals and advocates experienced a recent windfall: In 2015, the state Legislature disbursed a $2.2 million, three-year grant for pilot projects to address increasing HCV infections. Each of the five grantees set up different programs within their communities.
“When I first started this work a few years back, there were funding offers for testing, but it was like ‘Why?’” — Robert Lewis.
In San Francisco, the Department of Public Health worked to integrate primary care with specialized hepatitis C treatment. This included training primary care providers to handle more uncomplicated HCV cases, making sure vulnerable populations get access to testing and treatment, and creating an e-referral system to connect providers and pharmacists for rapid treatment of new diagnoses.
In more rural Butte County, the public health department focused on increasing confirmatory testing for new diagnoses.
Screening has become even more important now that there is effective treatment, according to Robert Lewis, director of special populations at the Family Health Centers of San Diego (FHCSD).
“When I first started this work a few years back, there were funding offers for testing, but it was like ‘Why?’” Lewis said. “We couldn’t treat them.”
Testing efforts are crucial both to provide treatment and contain infection: many people who have hepatitis C aren’t aware of their diagnosis, particularly those members of at-risk populations who don’t have access to regular healthcare.
A recent Oxford University study found in a large study of hepatitis C-infected young people that 80 percent lived more than 10 miles from the closest syringe service program.
Lewis added that one of the most effective ways of containing hepatitis C are Syringe Service Programs (or SSP). The state allocates $3 million annually in General Funds to operate the California Syringe Exchange Supply Clearinghouse, CDPH says.
But of California’s 58 counties, there are only 23 with access to syringe service programs, according to CDPH. This presents a major obstacle for preventing transmission of Hepatitis C.
A recent Oxford University study found in a large study of hepatitis C-infected young people that 80 percent lived more than 10 miles from the closest syringe service program. With so many of the people affected in rural counties, it could be the perfect storm for this outbreak to get worse.
That’s why the pilot grant program has been so crucial for the five grantees. As so many are federally qualified facilities, like the Family Health Centers of San Diego, or municipal public health departments, sparse funding is a constant problem.
“Hepatitis C is severely underfunded as a public health issue. That’s true nationally, and that’s true in California. — Katie Burk
“That’s the whole reason why we’re able to do the work that we’re doing and work with our community health care providers and our community itself,” said Cassie Miracle, Public Health Education Specialist Senior at Butte County Department of health. “We’re working with hospitals in Butte County to make those policy changes to make sure that everyone gets the testing that they need and to be quite frank, it’s worked so well!”
But even with the demo grant program, Burk and the other providers agree: money is still short.
“Hepatitis C is severely underfunded as a public health issue. That’s true nationally, and that’s true in California,” Burk said. “These demo projects are only going to five jurisdiction, but there’s huge need throughout the state. We could do so much more with more.”
The grant money runs out in June 2018.
One of those cuts could very well be a repeal of the ACA, an effort GOP lawmakers and President Trump have been doggedly pressing forward.
For now, no one is certain whether the programs it has funded in these five regions will continue. According to Miracle, grant recipients have been providing monthly and quarterly reports on their use of the funding, but she has heard nothing about the program’s future.
CDPH confirmed that the grant was not authorized beyond June 30, 2018, and evaluations of the program will be used to inform Hepatitis C prevention and treatment moving forward. While that grant’s demise presents one financial crisis for public health professionals fighting the transmission of Hepatitis C, there could be even more challenging policy changes on the horizon.
Though Republican efforts to repeal the Affordable Care Act are dead for now, any future efforts to repeal or just gut the program would have a major impact on those affected by this increase in Hepatitis C.
“We’re 100 percent reliant on people being covered by Medi-Cal, and Medi-Cal covering Hep C treatments,” Burk said. “The larger entities waiting for the other shoe to drop and understand how budget cuts are going to affect other priorities.”
One of those cuts could very well be a repeal of the ACA, an effort GOP lawmakers and President Trump have been doggedly pressing forward. While the most recent pushes failed, the threat looms over providers that depend on federal funding, like Medicaid reimbursements, would be hit hard. There is a major overlap between the people at risk for hepatitis C and those who rely on Medicaid or Medicare for health coverage. Many of the demo grant projects focused on providing testing and treatment to such underserved populations.
“Being a safety net provider for those who are underserved, there are times when there is a finite amount of money,” Tim Fraser, spokesperson for FHCSD said.
“Health centers are underfunded in a lot of places. A repeal of the ACA would be detrimental not only to the Hepatitis C facilities but to all health centers.”
Want to see more stories like this? Sign up for The Roundup, the free daily newsletter about California politics from the editors of Capitol Weekly. Stay up to date on the news you need to know.
Sign up below, then look for a confirmation email in your inbox.

Please share hope for those facing insurance access /denial problems. The barrier is the price, and a humanitarian Australian doctor has come up with a solution for the world- peaceful life saving and legal. Generic medication buyers club- saved my life and I admin a page, have seen 1000’s do it. I am a volunteer, trying to get the info to other people like me- this is legitimate, identical, look up the evidence- no denials of your civil right to import for yourself, it is about a grand. Please look up fixhepc as one word, check me out, but most of all please share- an American dies needlessly every 20 minutes because of the big pharma price.